generality
Il complement system it's a non-specific defense mechanism of the organism.
It is made up of numerous plasma proteins, which interact with each other and cooperate with other components of the immune system to eliminate foreign agents.
Complement proteins are normally present in the bloodstream, where - in the form of inactive precursors - they make up about 10% of globulins. Only in particular conditions (inflammation, infections or other pathologies), these precursors are activated; thus originate bioactive complexes responsible for the various biological effects, the most important of which is the cell lysis.
Complement proteins are made active by a set of enzymatic chain reactions, in a way very similar to what happens for the coagulation cascade: each component activates the next in the series, in defense of the organism.
Some diseases can lead to defects in the quantity and activity of complement proteins or their regulatory systems. The laboratory evaluation of these components makes it possible to measure their concentration in the bloodstream, as well as to verify their functionality. This test allows us to establish, therefore, if there are deficiencies or anomalies of complement proteins or their activity, such as to favor the onset of infections or increase autoimmune reactions (ie wrongly directed against the organism itself).
What's this
Complement is a set of plasma proteins, so called because it completes and integrates ("complements") the specific functions of antibodies.
The fundamental purpose of this system is to protect the organism, through the removal of pathogens (especially bacteria), interacting with immune complexes and / or facilitating their destruction by other biological systems, serum or cellular.
However, complement can also act in the absence of an antibody component. This system is activated, in fact, even in the presence of autoimmune diseases, in which antibodies are produced that react against organs and tissues belonging to the organism itself (autoantibodies).
Complement proteins: what are they?
- The complement system is made up of about thirty plasma proteins, which are flanked and regulated by numerous sub-components and inhibitors.
- The main complement proteins are 9 (C1-C9).
- Complement proteins interact according to a cascade model, which determines the formation of complexes capable of responding to infections, acting in inflammation and in cell death processes (apoptosis).
Pathways of complement activation
The complement is part of the defense mechanisms of theinnate immunity. Unlike the acquired one, which produces antibodies that recognize and protect the organism from specific aggressions, the innate immune system is non-specific.
This defensive mechanism is however very important, since it represents the first and fastest response that the human body implements if it detects potential pathogens.
The complement system does not require a preventive exposure to the foreign microorganism and does not keep memory of the substances with which it has previously come into contact.
The complement activation cascade can follow three ways:
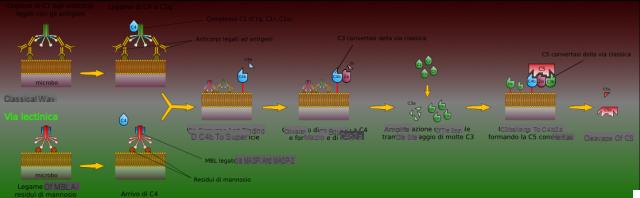
- Classic route: is that initiated by the formation of the antigen-antibody reaction, where the antigen can be an infectious agent (bacterium, virus, etc.), a cell or a protein foreign to the organism.
- Via alternatives: it does not depend on the presence of specific antibodies, but is activated directly by some components of the microbial surface;
- Via lectinica: it is triggered by a plasma lectin, following its binding to the mannose residues present on the microbial surface.
In all three pathways, the central event of complement activation is the proteolisi (cleavage) of the C3 protein. This event leads to the formation of biologically active products, which have the ability to attach themselves to the membrane of the cell that triggered the activation and to damage it, to the point of causing its destruction.
During the cascade, some "collateral" products are able to trigger a local inflammatory response (for example, they cause the release of histamine, increase the permeability of capillaries or the recall of white blood cells).
Because it is measured
The complement protein test allows you to measure its amount or activity in the blood.
To assess whether this defense system is functioning properly, its different components can be measured individually or as a whole.
Proteins C3 and C4 are the most frequently tested to determine if a particular pathological condition is caused by an alteration of the complement system.
Following the diagnosis of an acute or chronic condition involving this system, the test can be used to get a rough idea of the severity of the disease.
Testing for proteins C3 and C4 may also be requested occasionally if the clinician wishes to monitor the activity of a complement disorder.
When is the exam prescribed?
The doctor may indicate the evaluation of complement proteins in the presence of:
- Recurrent microbial infections (especially when they are of bacterial origin, such as those caused by Streptococcus pneumoniae, Neisseria meningitidis and Neisseria gonorrhoeae);
- Inflammation;
- Edema with no apparent cause;
- Symptoms associated with autoimmune disorders, such as systemic lupus erythematosus and rheumatoid arthritis.
- Diseases related to immune complexes such as glomerulo-nephritis, serum sickness and vasculitis (inflammation of the blood vessels).
The exam is also useful as an aid to monitoring an acute or chronic condition that involves alterations of the complement system.
The most frequently measured proteins are the C3 and C4 fractions. In the event that the clinician suspects the presence of a defect that cannot be highlighted with the measurement of these two components, the total activity of the complement can be measured (i.e. that concerning the 9 major glycoproteins, from C1 to C9).
If the total complement activity is outside the reference range, each of the nine different proteins that compose it can be measured individually, to identify any inherited or acquired deficits. In addition, evaluations of other components or inhibitors of the complement system (such as, for example, the C1 inhibitor) may be required to ascertain any abnormalities and identify decreased or increased components.
Normal Values
The examination of the complement protein activity involves the determination of two main fractions: the C3 and C4 fraction.
C3 fraction of the complement:
- Man: 80 - 185 mg / dl;
- Donna: 80 - 190 mg/dl.
C4 fraction of the complement:
- Man: 15 - 53 mg / dl;
- Donna: 15 - 57 mg/dl.
Note: the reference range of the exam may change according to the instrumentation used in the analysis laboratory. For this reason, it is preferable to consult the ranges reported directly on the report. It should also be remembered that the results of the analyzes must be evaluated as a whole by the general practitioner who knows the patient's medical history.
Causes of High Values
An increase in complement proteins can be found in:
- Autoimmune diseases;
- Inflammations (including ulcerative colitis and thyroiditis);
- Chronic infections;
- Cancer (leukemia, Hodgkin's lymphoma, sarcoma, etc.);
- Acute myocardial infarction;
- Sarcoidosi;
- Juvenile rheumatoid arthritis.
Causes of Low Values
Complement proteins are reduced under the following conditions:
- Liver diseases (acute and chronic hepatitis, cirrhosis, etc.);
- Nephropathy (including glomerular nephritis, lupus nephritis, membranous nephritis, IgA nephropathy, and renal failure);
- Enteropathy protidodisperdenti (coliti);
- Malnutrition;
- Burns;
- collagenopathy;
- Idiopathic autoimmune haemolytic anemia.
Decreased complement levels can also be observed in the presence of:
- Recurrent microbial infections (mostly bacterial);
- Autoimmune diseases, such as systemic lupus erythematosus (SLE) and rheumatoid arthritis;
- Hereditary or acquired angioedema;
- Septicemia;
- Serum sickness (immune complex mediated hypersensitivity).
How it is measured
Since these are detectable proteins in the bloodstream, the complement system can be evaluated by taking a blood sample from a vein in the arm.
Preparation
Before undergoing the examination of complement proteins, it is necessary to observe a fast of at least 8 hours, during which a moderate amount of water is allowed.
Interpretation of Results
The increase or decrease in the levels of complement proteins does not allow the diagnosis of the specific pathology affecting a patient, but does provide indications regarding the involvement of the immune system.
Complement Proteins - Low Values
Complement levels can decrease in the presence of:
- Congenital deficit of one of the complement proteins (relatively rare condition). As a rule, this is associated with recurrent infections.
- Increased consumption, as can occur in a number of inflammatory and infectious diseases (rheumatoid arthritis, SLE, subacute bacterial endocarditis, immunocomplex diseases, etc.).
If the deficiency is caused by an underlying acute or chronic disease, complement levels usually return to normal as soon as the triggering condition itself is resolved.
Decreased complement levels are associated with an increased risk of developing autoimmune disorders.
Usually, both C3 and C4 values are decreased in systemic lupus erythematosus; in the course of septicemia and infections caused by fungi or parasites (such as malaria), however, only the levels of C3 decreased.
Complement Proteins - High Values
Complement values are typically increased in chronic or acute inflammation (C3 and C4 behave like "acute phase" proteins). Levels of these proteins return to normal following resolution of the disease.
An increase in complement proteins can also be found in the context of rheumatic fever, viral hepatitis, myocardial infarction, malignant tumors, diabetes, thyroiditis, gastrointestinal inflammatory diseases and various infectious diseases.


























