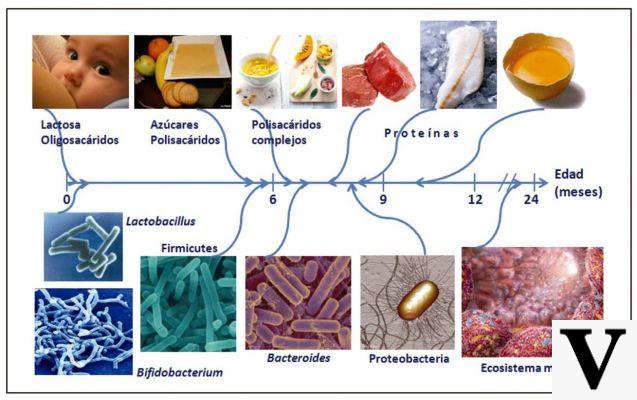
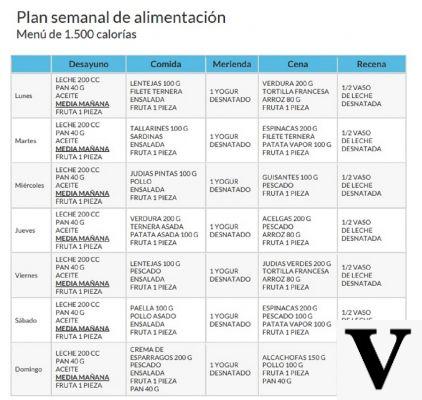
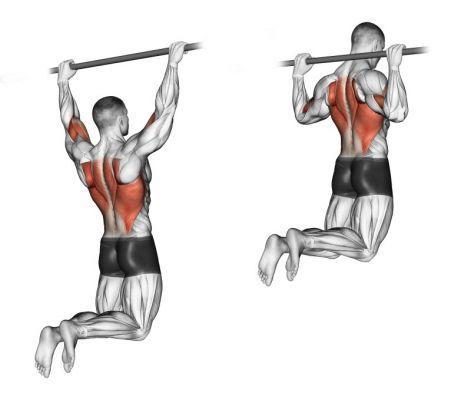
What's this
What is Vitamin D
Vitamin D is a group of fat-soluble secosteroids necessary for the intestinal absorption of minerals such as calcium, magnesium and phosphate, and for many other biological functions.
In humans, the most important compounds in this group are vitamin D3 (also known as cholecalciferol) and vitamin D2 (known as ergocalciferol) - which however will need to be mutated into calcitriol (the active hormonal form).
The main natural source of vitamin D is constituted by the endogenous production of cholecalciferol (vit D3) in the skin, starting from cholesterol, through a chemical reaction that depends on exposure to sunlight (in particular from UVB irradiation). However, cholecalciferol and ergocalciferol can also be taken with the diet and supplements, but only a few foods can be considered good sources of vitamin D (especially fish, liver and egg yolk; secondly, certain mushrooms as well).
Dietary recommendations for vitamin D have a large margin of safety and generally do not take into account the extent of sun exposure, relying entirely on nutritional intake. This is because, by virtue of the variability linked to the different latitudes (hours of light and darkness are seen in the Nordic countries), the uptake of UVB rays in the population is rather variable; What's more, let's not forget that excessive sun exposure can increase the risk of skin cancer.
Both vitamin D introduced with food and that produced in the skin are biologically DON'T active and necessarily require the intervention of a protein enzyme capable of hydroxylating them by converting them into the biologically active form. This occurs in the liver and kidneys. Since vitamin D can be synthesized in adequate quantities by most mammals sufficiently exposed to sunlight, DON'T it should be considered an essential dietary factor - so it shouldn't even be considered a vitamin. Rather, it has the characteristics of a prohormone, which can be activated in the hormone calcitriol, which produces its effects by interacting with a nuclear receptor located in several cells of different tissues.
Cholecalciferol (vit D3) is converted to calcifediol (25-hydroxycholecalciferol), while ergocalciferol (vit D2) is converted to 25-hydroxyergocalciferol. These two metabolites of vitamin D (called "25-hydroxyvitamin D" or "25 (OH) D") can be measured in the blood serum to determine a person's total vitamin D level. Calcifediol is then further hydroxylated by the kidneys to form calcitriol (also known as "1,25-dihydroxycholecalciferol"), the biologically active form of vitamin D. Calcitriol circulates as a real hormone in the blood, playing a very important role in homeostasis and in the metabolism of calcium and phosphate, regulating their concentrations in the blood and promoting physiological growth of the skeleton, bone remodeling and preventing degeneration with old age. Calcitriol also has other biological effects, including a role on cell growth, various neuromuscular and immune functions, and reducing inflammation.
The discovery of vitamin D came with the search for the missing dietary substance in children with rickets (the infantile form of osteomalacia). Vitamin D supplements are therefore given to treat or prevent osteomalacia, rickets and osteoporosis, but there is little or no scientific evidence for other health effects in the general population. The effect of vitamin D supplementation on mortality is not yet fully understood, although almost all research groups agree that there is no justification for recommending supplementation for preventive purposes for various diseases.
Professional Chermisty
Structure and chemistry of vitamin D.
The term vitamin D refers to all secosteroids (steroids in which one of the bonds in the steroid rings is open) which have the biological activity of calciferol and are characterized by being derivatives of cyclopentanoperhydrophenanthrene. There are several forms, of which the main ones are two: vitamin D2 or ergocalciferol and vitamin D3 or cholecalciferol. The structural difference between vitamin D2 and vitamin D3 is that the side chain of D2 contains a double bond between carbons 22 and 23 and a methyl group on carbon 24.
For further information: Skin synthesis of Vitamin DCalciferol is 50-100 times more active than ergocalciferol (D3 is more active than D2). Both ergocalciferol and calciferol are inactive forms of vitamin D, therefore activation is required in the liver and kidneys. Man is able to synthesize cholecalciferol starting from a precursor, with the function of provitamin: dehydrocholesterol (derived from cholesterol by reduction). This provitamin is found in the skin, so it absorbs the solar radiation energy that causes isomerization to cholecalciferol (see skin synthesis of vitamin D). Adequate sun exposure therefore reduces the need for vitamin D.
Note: speaking of vitamin D or calciferol, without specifying any reference index, we mean vit D2 or vit D3 or both. Vitamin D2 was differentiated in 1931 while, after irradiation of 7-dehydrocholesterol, vitamin D3 was discovered in 1935.
Biology
Biology of Vitamin D
The active metabolite of vitamin D (calcitriol) exerts its biological effects by binding to the vitamin D receptor (VDR), which is found mainly in the nucleus of target cells. The binding of calcitriol to the VDR allows it to act as a transcription factor that modulates the gene expression of transport proteins (for example TRPV6 and calbindin), in turn involved in the absorption of calcium in the intestine. The vitamin D receptor belongs to the superfamily of steroid / thyroid hormone receptors and is expressed by cells in most organs, including: brain, heart, skin, gonads, prostate and breast.
Activation of VDR in intestinal, bone, kidney and parathyroid cells leads to the maintenance of calcium and phosphorus levels in the blood (with the help of parathyroid hormone and calcitonin) and the preservation of bone content.
One of the most important roles of vitamin D is maintaining skeletal calcium balance, promoting calcium absorption in the intestine, bone resorption by increasing the number of osteoclasts, maintaining calcium and phosphate levels for bone formation and allowing parathyroid hormone to function properly to maintain serum calcium levels. Vitamin D deficiency can lead to lower bone mineral density and an increased risk of reduced bone density (osteoporosis) or bone fracture, because a lack of vitamin D alters mineral metabolism in the body. Therefore, vitamin D is also essential for bone remodeling through its role as a powerful reabsorption stimulator.
VDR also regulates cell proliferation and differentiation. Vitamin D also interacts with the immune system, and VDRs are expressed in several types of white blood cells, including monocytes and activated T and B cells. In vitro, vitamin D increases the expression of the tyrosine hydroxylase gene in adrenal medullary cells and influences the synthesis of neurotrophic factors, nitric oxide synthase and glutathione.
functions
What is Vitamin D used for?
Calciferol acts with a hormone-like mechanism of action, as:
- It is synthesized autonomously by the human organism
- It acts on a target organ
- It has a structure that resembles steroid hormones.
Vitamin D is essential for calcium and phosphate homeostasis, and is crucial for the growth and maintenance of the skeleton. The metabolically active form is 1,25- (OH) 2-cholecalciferol, which acts by favoring:
- Absorption of calcium and phosphate in the intestine
- Deposition of calcium from bones
- Maintenance of cartilage trophism
- Renal reabsorption of calcium and phosphorus in the proximal convoluted tubule.
Vitamin D and calcium
1,25- (OH) 2-cholecalciferol stimulates the synthesis of CaBP (calcium-carrying protein) in the target organ (enterocytes), intervening at the level of the intestinal DNA transcription that encodes the protein and plasma RNA polymerase . The use of actinomycin D and a-amanitin inhibitors of transcription and RNA polymerase, respectively, confirm this action. In this way new RNA is synthesized which favors the synthesis of CaBP necessary to favor the absorption of calcium. It is now certain that cyclic AMP is involved in this process, which increases in the tissues by the action of active vitamin D.
Food Sources
Where is Vitamin D found?
The foods richest in vitamin D are: liver, fish oil, marine fish (herring, salmon, sardine) and egg yolk; smaller quantities are present in mushrooms.
For further information: Where is itNote: almost all of vitamin D is synthesized in the skin; adequate exposure to the sun is therefore recommended, especially for the elderly.
For further information: Vitamin D in FoodsVitamin D: how to take it
The health benefits of vitamin D supplementation are uncertain. A 2013 review found no effect of integration on disease rates, other than a XNUMX-year decrease in mortality in the elderly. Vitamin D supplements do not alter outcomes for myocardial infarction, stroke or cerebrovascular disease, cancer, bone fractures, or osteoarthritis of the knee. Low vitamin D levels can result from a disease rather than the cause of it.
A report from the "United States Institute of Medicine" states: "Outcomes related to cancer, cardiovascular disease and hypertension, diabetes and metabolic syndrome, falls, immune efficiency and autoimmune diseases, infections, neuropsychological functioning and preeclampsia cannot be reliably linked. to the intake of calcium or vitamin D and are often conflicting ".
For further information: Vitamin D supplementsVitamin D3 Rite-Flex Supplement
The Rite-Flex vitamin D3 supplement is designed to support the proper functioning of the immune system and promote the well-being of the skeletal and muscular system. Among other benefits, this Rite-Flex supplement contributes to the maintenance of calcium levels in the blood. These soft tablets do not contain gluten, lactose, soy or GMO ingredients; they do not contain artificial flavors or aggressive chemicals. The main ingredient is sunflower oil, while the capsule shell is made with glycerin, gelatin and water.
 Rite-Flex Vitamin D3 2000IU (50μg) for bone support - joint and immune system | Non-GMO and gluten-free from 2X to 2.000 IU - 365 easy to swallow softgels from
Rite-Flex Vitamin D3 2000IU (50μg) for bone support - joint and immune system | Non-GMO and gluten-free from 2X to 2.000 IU - 365 easy to swallow softgels from
 € 18,90 Check out the offer
€ 18,90 Check out the offer
Vitamin D supplement by Yamamoto Nutrition
Vitamin D is a vitamin D supplement to be used in case of reduced intake of this particular vitamin with the diet or due to increased needs of the organism. This supplement promotes the well-being of hair, teeth, bones and skin. The package contains 90 capsules and each in turn contains 25 grams of vitamin D. The indication on the package says to take one tablet a day but, as with other supplements, it is always good to ask the doctor's opinion.
 Vitamin D 25mcg Vitamin D food supplement 90 capsules of
Vitamin D 25mcg Vitamin D food supplement 90 capsules of
 € 11,93 Check out the offer
€ 11,93 Check out the offer
Absorption
Absorption of vitamin D
Calciferol is absorbed in the intestine in the same way as lipids: it then becomes part of the micelles (which are formed by combining bile salts with products deriving from lipid hydrolysis), is absorbed by passive diffusion in the enterocytes and subsequently incorporated in the chylomicrons and transported through the mesenteric lymphatic vessels. Unlike other fat-soluble vitamins, calciferol is not stored in the liver. However, the amount of calciferol from food is very low and most of vitamin D is synthesized in the skin by the action of ultraviolet light.
Need
Vitamin D requirement
Under normal conditions, exposure to sunlight is sufficient to meet the body's needs for calciferol. However, especially for safety, the following levels of intake are recommended in your country:
- infants 10 ÷ 25 µg
- children 1 ÷ 3 years 10 µg
- children 4 ÷ 10 years 0 ÷ 10 µg
- girls and boys 11 ÷ 17 years 0 ÷ 15 µg
- adulti 0÷10 µg
- elderly 10 µg
- pregnant 10 µg; nutrice 10 µg.
Note:
- 1 IU = 0,025 µg of calciferol
- 1 µg of calciferol = 40 IU of vitamin D.
Below are tables of recommended levels in the United States, Canada, Australia, New Zealand and the European Food Safety Authority.
For further information: Vitamin D: Requirement| United States | ||
| Age | RDA (IU / die) | mcg / die |
| Babies 0-6 months | 400* | 10 |
| Babies 6-12 months | 400* | 10 |
| 1 70-years | 600 | 15 |
| over 70 years | 800 | 20 |
| Pregnant and nursing | 600 | 15 |
| Age | Maximum tolerable dose (IU / day) | mcg / die |
| Babies 0-6 months | 1000 | 25 |
| Babies 6-12 months | 1500 | 37,5 |
| Children 1-3 years | 2500 | 62,5 |
| Children 4-8 years | 3000 | 75 |
| over 9 years | 4000 | 100 |
| Pregnant and nursing | 4000 | 100 |
| Canada | ||
| Age | RDA (IU) | Maximum Tolerable Dose (IU) |
| Babies 0-6 months | 400* | 1000 |
| Babies 7-12 months | 400* | 1500 |
| Children 1-3 years | 600 | 2500 |
| Children 4-8 years | 600 | 3000 |
| children and adults 9-70 years | 600 | 4000 |
| over 70 years | 800 | 4000 |
| Pregnant and nursing | 600 | 4000 |
| Australia and New Zealand | ||
| Age | Adequate intake (mcg) | Maximum tolerable dose (mcg) |
| Babies 0-12 months | 5* | 25 |
| Children 1-18 years | 5* | 80 |
| Adults 19-50 years old | 5* | 80 |
| Adults 51-70 years old | 10* | 80 |
| Adults over 70 years old | 15* | 80 |
| European Food Safety Authority | ||
| Age | Adequate intake (mcg) | Maximum tolerable dose (mcg) |
| Babies 0-12 months | 10 | 25 |
| Children 1-10 years | 15 | 50 |
| Children 11-17 years | 15 | 100 |
| Adults | 15 | 100 |
| Pregnant and nursing | 15 | 100 |
| * Adequate intake, no RDA / RDI established | ||
Shortage
Vitamin D deficiency: when to worry?
For further information: Vitamin D deficiencyA real deficiency of this vitamin can be assessed with blood tests, and confirmed by low concentrations.
A diet lacking in vitamin D in combination with inadequate sun exposure causes osteomalacia in adults and rickets in children, which consist in the rarefaction of bone tissue. In the Western world, these conditions are very rare today. However, vitamin D deficiency has become a worldwide problem for the elderly population and remains common in children and adults in less developed countries. The low content of calcifediol (25-hydroxy-vitamin D) derives mainly from a poor sun exposure. The deficiency leads to reduced bone mineralization and damage to the skeleton leading to the aforementioned diseases. Having a vitamin D deficiency can reduce intestinal absorption of calcium to only 15%. When not deficient, an individual usually absorbs between 60-80% of dietary calcium.
Vitamin D and bone health
Vitamin D and rickets
Rickets, typical of childhood, is a disease characterized by reduced growth and long, soft, weak and deformed bones - which bend under weight when children begin to walk. This condition, typically characterized by the bowing of the femurs outward, can be caused by a lack of calcium and / or phosphorus, as well as a lack of vitamin D; today it is widespread in most low-income countries such as Africa, Asia or the Middle East, or in people with genetic disorders such as pseudovitamina D deficiency.
Vitamin D deficiency in the mother can cause bone disease manifested before birth and impaired skeletal quality after birth. Nutritional rickets is typical of countries with intense sunlight throughout the year, such as Nigeria, and can also occur without vitamin D deficiency (for example due to calcium and phosphorus deficiency).
Although rickets and osteomalacia are now rare in the UK, outbreaks have occurred in some immigrant communities in which women with seemingly adequate exposure to daylight wore particularly opaque clothing. Darker skin and reduced sun exposure do not usually lead to rickets, unless the diet deviates from the Western omnivore pattern characterized by high intakes of meat, fish and eggs. The major dietary risk factor for rickets includes elimination from animal foods - as occurs in the vegan diet.
Vitamin D deficiency remains the leading cause of rickets among young children in most countries because breast milk is poor of vitamin D, and why social habits and climatic conditions can prevent adequate sun exposure. In sunny countries like Nigeria, South Africa and Bangladesh, where rickets occurs in young and old children, an inadequate level of calcium - typical of grain-based diets with a shortage of dairy products - is most responsible.
In the past, rickets has been a major public health problem; in Denver (USA), for example, where ultraviolet rays are about 20% stronger than sea level at the same latitude, nearly two-thirds of 500 children had mild rickets in the late 20s. . An increase in the proportion of animal and plant proteins in the XNUMXth century American diet, coupled with the increase in the consumption of vitamin D-fortified milk, coincided with a drastic decline in the number of cases of rickets. Additionally, in the United States and Canada, vitamin D-fortified milk, infant vitamin supplements, and vitamin supplements have helped eradicate most cases of rickets for children with specific fat malabsorption.
Vitamin D, osteoporosis and osteomalacia
Osteomalacia is an adult disease that results from vitamin D deficiency. Characteristics of this disease are softening of the bones, leading to flexion of the spine, bowing of the legs, proximal muscle weakness, bone fragility and an increased risk of fractures. Osteomalacia reduces calcium absorption and increases bone demineralization, increasing the risk of fractures; it usually appears when 25-hydroxyvitamin D levels are below approximately 10 ng / mL. Although it is conceivable that the effects of osteomalacia contribute to chronic musculoskeletal pain, there is no persuasive evidence that low levels of vitamin D are responsible for chronic pain, or that supplementing it can alleviate it.
Vitamin D and skin pigmentation
Dark-skinned people living in temperate climates have been shown to have low levels of vitamin D, probably due to a lower efficiency in its production caused by the abundant melanin in the skin, which would hinder the synthesis of the same.
Signs of vitamin D deficiency
The early signs of calciferol deficiency are:
- serum reduction of calcium and phosphorus
- secondary hyperparathyroidism and increased serum alkaline phosphatase.
Later signs are:
- inadequate mineralization of the skeleton (rickets in children, osteomalacia in adults)
- muscle weakness
- abdominal pain.
Rickets appears in children between 4 and 24 months of age and basically consists of inadequate mineralization of the growing bone, which leads to skeletal deformations.
In the first months of life, the symptoms essentially concern the skull with:
- softening in the occipital, temporal and parietal regions
- delay in closing the anterior fontanel (becomes pathological after the fifteenth month of life)
- rachitic rosary (between the sixth and twelfth month) hypertrophy of the chondro-costal junctions
- hypertrophy of cartilage (in older children) with knots especially in the wrists and ankles
- bowing of the long bones of the lower limbs and valgus knee.
Osteomalacia occurs in adults with:
- muscle weakness
- pain in the back-lumbar tract of the spine, pelvic girdle and thighs
- insecure gait and bone fragility, especially of the spine, shoulders, ribs and pelvis
- extremely low bone density and presence of pseudo-fractures, especially in the spine, femur and humerus (detectable on x-ray)
- increased risk of fractures especially in the pelvis and wrists.
Toxicity
Vitamin D toxicity
Cases of vitamin D toxicity are rare and caused by supplementing with high doses of vitamin D - not food or excessive sun exposure. The threshold for vitamin D toxicity has not yet been established; however, according to some research, the Tolerable Upper Intake Level (UL) would be 4.000 IU / day for ages 9-71 (100 μg / day); other insights, however, conclude that, in healthy adults, the prolonged intake of 1250 μg / day (50.000 IU) can produce evident toxicity after several months and increasing the serum levels of 25-hydroxyvitamin D to 150 ng / mL and beyond. Those with certain medical conditions, such as primary hyperparathyroidism, are much more sensitive to vitamin D and develop hypercalcemia in response to any increase in vitamin D, while maternal hypercalcemia during pregnancy can increase sensitivity to mental retardation and deformity syndromes. face them.
A review published in 2015 found that adverse effects were only reported at serum concentrations of 25 (OH) D above 200 nmol / L.
Published cases of toxicity involving hypercalcaemia in which vitamin D dose and 25-hydroxy-vitamin D levels are known all result in consumption of ≥40.000 IU (1.000 μg) per day.
Pregnant or nursing women should consult their doctor before taking a vitamin D supplement. The Food and Drug Administration (FDA) has advised manufacturers of liquid vitamin D supplements to include a dropper marked for 400 international units ( 1 IU is the biological equivalent of 25 ng cholecalciferol / ergocalciferol). Also, for products intended for infants, the FDA recommends that the dropper contain no more than 400 IU. For infants (from birth to 12 months), the tolerable upper limit (maximum amount that can be tolerated without harm) is set at 25 μg / day (1.000 IU). A thousand micrograms a day in babies produces toxicity within a month. After being commissioned by the Canadian and American government, the Institute of Medicine (IOM) has increased the upper tolerable limit (UL) to 2.500 IU per day for ages 1-3 years, 3.000 IU per day for ages 4-8 years and 4.000 IU per day for ages 9 to 71 (including pregnant or lactating women).
Calcitriol concentration is self-regulated by a negative feedback loop and is also influenced by parathyroid hormone, fibroblast growth factor 23, cytokines, calcium and phosphate.
Signs and symptoms of excess vitamin D.
Hypervitaminosis (excess vitamin D) causes increased intestinal absorption and bone resorption of calcium, resulting in hypercalcemia, easily identifiable due to increased urination and thirst.
If left untreated, hypercalcemia results in excess calcium deposits in soft tissues and organs such as the kidneys, liver and heart, causing pain and organ damage. This is associated with the decrease in serum PTH (quantity of parathyroid hormone present in the blood, see: calcium and osteoporosis) and finally loss of calcium homeostasis with consequent:
- anorexia, nausea, vomiting and diarrhea
- ipercalcemia and ipercalciuria
- nephrocalcinosis, cardiocalcinosis and soft tissue calcification.
These can be followed by polyuria, polydipsia, weakness, insomnia, nervousness, itching and eventually kidney failure. In addition, proteinuria, urinary stones, BUN, and metastatic calcification (especially in the kidneys) may develop. Other symptoms of vitamin D toxicity include mental retardation in young children, abnormal bone growth and formation, diarrhea, irritability, weight loss, and severe depression.
Vitamin D toxicity is treated by stopping vitamin D supplementation and limiting calcium intake. Kidney damage can be irreversible. Exposure to sunlight for long periods of time does not normally cause vitamin D toxicity. Concentrations of vitamin D precursors produced in the skin reach a balance and any further production is degraded.
Excessive intake of calciferol in the diet is extremely unlikely, given the reduced amount of vitamin D in food; just as there are no known cases of hypervitaminosis due to excessive exposure to the sun. On the other hand, intoxication is possible following the administration of calciferol for therapeutic purposes.
Sponsored Content: healthiergang.com features products and services that can be purchased online on Amazon and / or other e-commerce sites. Whenever a purchase is made through one of the links on the page, healthiergang.com could receive a commission from Amazon or from the other e-commerce companies mentioned. We inform you that the prices and availability of the products are not updated in real time and may change over time, so we invite you to check availability and price on Amazon and / or on other e-commerce mentioned.