Introduction
The relationship between irritable colon (IBS) and diet is certainly very strong.
That said, curiously, recent theories suggest that nutrition is actually DON'T lva considered to be the main cause of irritable bowel, but rather a factor that it can exacerbate it o sharpen it symptoms and clinical signs.
The etiology of IBS could be totally different, more precisely linked to a different one nervous communication between brain and intestine. We speak of "difference" and not of "defect" since, to date, irritable bowel syndrome is not considered a disease.
Indeed, many other factors have an impact; for example the psychological state, other elements that can chemically irritate the intestine (spicy foods, alcohol, nerves, etc.), any comorbidities such as diverticula, digestive enzymatic deficiencies, etc.
From what has been said, however, it emerges that the only factors manageable are those of dietary relevance - even if many subjects report great improvements following anxiolytic, pharmacological or psychological-behavioral therapy.
On balance, people with intense symptoms often don't understand what to eat to improve your condition. In this article we will try to better understand how to set the most suitable diet therapy
For further information: Irritable Colon Syndrome: What is it? Causes
Irritable Colon
Irritable bowel syndrome, or more specifically irritable bowel syndrome (SSI) / irritable bowel syndrome / irritable bowel syndrome (IBS), is among the most common gastrointestinal functional disorders (DFGI) in the general population.
What is there to know about irritable bowel?
Irritable bowel syndrome is a disorder that affects the final portion of the large intestine, where the absorption / reabsorption of fluids and minerals from the stool is completed.
The irritable bowel is characterized by a rather generic clinical picture, with symptoms that DON'T they depend on pathological changes in the organ. It essentially manifests itself with abdominal pain, bloating, abdominal swelling and tension, and changes in the hollow (constipation or constipation, diarrhea) - also mixed.
Although causing manifestations of rather significant intensity, the irritable bowel syndrome DON'T it is to be considered a real disease but rather an uncomfortable condition - contrary ulcerative colitis, Crohn's disease, which imply an inflammatory state, and diverticulitis, which is based on the infection of the diverticula.
IBS must also be differentiated from intolerances (lactose, celiac disease, non-celiac gluten sensitivity, etc.) or certain food allergies properly called and diagnosable.
Not for nothing, its diagnosis is almost always "exclusion" with respect to organic diseases from which it must be differentiated.
Contrary to popular belief, the differential diagnosis of irritable bowel syndrome is very important; this is because some diseases of the intestine - some almost harmless, others serious - can manifest themselves with very similar symptoms; it is therefore worthwhile to perform all the necessary tests to exclude these pathological conditions.
In any case, anyone who experiences such symptoms - we repeat: abdominal pain, constipation and / or diarrhea - should not be too alarmed; but don't underestimate the question either.
It should be borne in mind that, boasting an incidence between 10-20 % circa - of which the 70 % consisting of women - irritable bowel syndrome constitutes intestinal discomfort most widespread throughout the West e absolutely DON'T related the incidence of colorectal cancer.
In the absence of a clearly discernible cause, IBS is often associated with impaired psychological stability.
The pathogenetic mechanism is controversial and still completely lacking in adequate scientific confirmation.
On the other hand, it is possible that the colon, being provided with its own neuro-hormonal regulation but related to the brain, is the object of dysfunctions affecting the release or uptake of certain chemical mediators.
Some mechanisms likely to be compromised by irritable bowel syndrome are:
- alteration of the release of serotonin (responsible, among other things, for smooth muscle contraction);
- capillary vasoconstriction;
- immune regulation of the mucosa.
In practice, brain activity changes the intestinal one and can give rise to irritable bowel syndrome.
Other mechanisms "theoretically" able to contribute, activate or worsen irritable bowel syndrome are the nerve modifications that affect intestinal contractility and visceral hyperalgesia (ie increased sensitivity to pain).
However, it cannot be ruled out that irritable bowel syndrome may depend on other still unknown factors such as, for example, the inflammation typical of certain colitis.
Especially for its multifactorial etiology, with nutritional, nervous, sometimes idiopathic factors, IBS it cannot be cured in the strict sense of the term, but rather prevented o compensated making it asymptomatic.
It follows that the treatment of irritable bowel syndrome itself must be highly specific and multidisciplinary.
On the other hand, diet is certainly a determining factor; it could be argued that dietary therapy, combined with the management of nervous stress, is the only omnipresent element in the therapy of this syndrome.
For further information: Irritable Colon Syndrome: DiagnosisTreatment
As we have said, the diet is not to be considered a real cause of irritable bowel syndrome, but it still represents a decisive element in its treatment - necessary for the moderation of symptoms.
According to the clinical experience of many professionals, irritable bowel syndrome appears to significantly improve with the patient's emotional balance. This happens both in occasional circumstances - such as the holiday period - and in conjunction with certain anxiolytic drug therapies. That said, it is not possible to stay on vacation all the time and not even take anxiolytics just to improve the condition of your alvo.
This is why it is essential to act in a multifactorial way, first of all by regularizing the lifestyle, reducing the load of nervous stress and carrying out motor activities systematically - necessary to fight the primary cause - but also dedicating the time and energy necessary to managing the diet - essential to reduce symptoms.
For further information: Cure Irritable Colon Syndrome: Which TreatmentDiet
The irritable bowel diet is essential to moderate the frequency and intensity of symptoms.
On the other hand, DON'T it's possible standardize totally the therapeutic system, as the alteration of the hive can be diametrically opposite depending on the case.
The prevalence of the type of alteration oftarget, or the differentiation between constipation and diarrhea, is an aspect that is far from negligible.
While the constipation mainly affects the women, disastrous too liquid they manifest themselves mainly in the male sex - even if sometimes the two symptoms alternate with a prevalence of one or the other component.
It is true that, if we considered the intestine of "normal" people, in both circumstances we could benefit from the increase in the share of soluble fibers. Yet, field experience has shown that this component is often not effective in the resolutive treatment of symptoms.
Many people get good results eliminating all the products virtually "irritants" or stimulants, such as alcohol, coffee, cigarette smoke, and spicy foods. Even in this case, however, results are not always guaranteed.
The use of probiotic supplements it is quite controversial, in the sense that for some it leads to some improvements, while for others it seems even negative.
Following some in-depth studies, a factor emerged that, for many, proved to be decisive. The correlation between the symptoms of IBS and the presence of some details carbohydrates which would appear to have a strong trend to the fermentation.
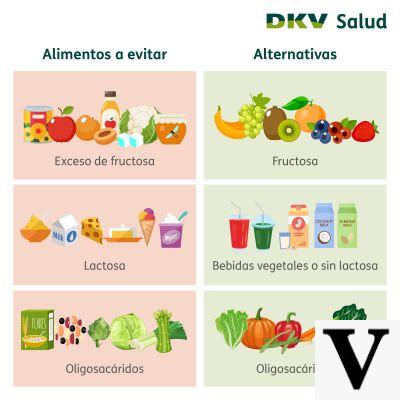
We are talking about molecules, both available and unavailable for human digestion, belonging to the categories: oligosaccaridi, disaccharides, monosaccaridi e polyol. Therefore, some would also have an energetic function for our organism, while others act as dietary fiber or in any case as a prebiotic.
The nutritional system that searches for and excludes these elements is said Low-FODMAPs Diet. In practice, it has shown some success but which, however, does not concern all patients (coverage has reached about 2/3). Furthermore, sensitivity to FODMAPs is often selective, subjective and dose dependent.
L'association of all the recommendations cited above it is, in all likelihood, the best dietary combination against irritable bowel.
Let's go into more detail.
What to eat in the diet for irritable bowel with constipation or constipation?
Over 70% of cases of irritable bowel syndrome affect women; consequently, the predominant picture is certainly constipation associated with intestinal pain, a sense of relief after evacuation and, sometimes, perception of progressive increase in abdominal circumference (feeling of bloating from abdominal tension), with hints of excessive fullness; often, people affected by irritable bowel syndrome with constipation also complain of goat stools, incomplete emptying, hemorrhoids and / or fissures.
In irritable bowel syndrome with constipation, more fiber and more water are generally needed, other laxative foods such as kiwis and probiotic factors can also help.
However, unlike constipation primarily due to a lack of fiber and water in the diet, constipation associated with irritable bowel syndrome DON'T it is directly related to these two nutritional components; having said that, these can certainly affect symptoms.
It is important to keep in mind that the severity, so to speak, of the manifestations can have multiple etiology, consequently it can benefit from even different dietary and / or behavioral corrections.
Moreover, the fact that there is no direct correlation with these two dietary elements indicates that, usually, even the intake of 30 g of fiber and 1,5-2 liters of water per day DON'T manages to normalize intestinal function.
The intake of probiotics associated with prebiotics is sometimes positive on symptoms. However, this is a weak correlation, but worthy of consideration.
Even the exclusion of FODMAPs can, paradoxically, reduce constipation. Although some of these molecules are fermentable by the bacterial hole, an excessive activity of the latter can inflate the intestine and irritate it, or in any case promote a contraction that is unfavorable to the progress of the stool. This would explain why some constipated people, by reducing some foods of plant origin - and replacing them with others - obtain improvements on the symptom.
Nutritional therapy is however indispensable to differentiate diet-dependent constipation from psychogenic irritable bowel syndrome.
What to eat in the diet for irritable bowel with diarrhea?
If it is true that in irritable bowel syndrome with constipation the increase in fibers and water does not necessarily lead to an improvement in bowel movements, in the case of diarrhea the speech becomes even more complicated.
In a simplistic way we could recommend:
- increase the fibers soluble - because they are able to gel the residual water in the intestinal lumen;
- limit those insoluble - which tend to increase gases and peristaltic contractions, therefore also meteorism;
- and try to to exclude:
- the factors anti-nutritional - such as protease inhibitors, oxalates, phytates;
- the elements osmotici - such as lactulose in hot milk;
- the irritants - including nerves such as alcohol and caffeine;
- the spices spicy like chilli and pepper;
- i FODMAP subject of hypersensitivity - read the dedicated article by clicking here.
- i big glycemic loads, such as pizza etc.
- Sfare beware of probiotics; if for some they demonstrate a positive effect, perhaps empowering greater health the mucosa in the case of - however more often compromised in the forms of pathological diarrhea - for others they aggravate the symptoms.
We haven't talked about water. This is because it is not recommended to reduce your water intake with food and drink, as it always is necessary to the proper functioning of the organism. It is not even possible to manage intestinal reabsorption, because diarrhea itself it is a form of malabsorption of liquids.
Also it seems that even fasting, therefore drastically reducing the intake of liquids - with the diet we assume most of the daily water - dthe persistence persists evolvendosi in mucorrea - prevalence of mucus compared to the faeces themselves. Sometimes, the frequency of bowel movements in irritable bowel with diarrhea is so high that it causes mucorrhea even without fasting.
It is advisable to give up foods rich in insoluble fiber, or the parts of the same that contain them; in fact, insoluble fibers often abound in the peel of vegetables, fruit, in the outer portion to the semi starchy such as cereals (bran) and legumes etc.
It turns out however inadvisable practice a low residue diet, as the soluble fibers have a gelling action.
It can be an excellent habit to prefer, in moments of acuity, i cooked vegetables but poor in FODMAP - cooking improves fiber solubility - and peeling - for the above reasons.
Irritable colon is a lot widespread also in subjects in overweight. In this regard, we remind you that among the various functions of fibers, in addition to those of stimulus area of peristalsis intestinal and prebiotic, there is also the favor of satiety.
For further information: FODMAP Diet for the Irritable Colon: How It Works and EffectivenessFood Intolerances VS Irritable Colon
The fact that it comes to the diagnosis of irritable bowel syndrome for exclusion, it can hide certain situations of a quite different nature. This is the case, for example, of lactose food intolerances and gluten sensitivity.
These two conditions, usually diagnosable with specific tests, are sometimes almost impossible to recognize. In these cases, the first investigations can give false negative results, convincing the doctor that the patient is not intolerant (when in reality he is) and orienting him towards the diagnosis of irritable bowel (actually absent). Therefore, it is always advisable to carry out all the diagnostic paths of the case and implement (with the help of a dietician) a diet "of exclusion"useful for recognizing any intolerances responsible for the symptoms.
For example, every source of gluten could be eliminated from the diet for a few weeks - from two weeks to a couple of months - evaluating any improvements and, if not present, also proceeding to exclude the major sources of lactose. Be careful though, any positive effect must be analyzed in its entirety. Sometimes the exclusion of gluten results in the elimination of complex carbohydrates. This often leads to a reduction in total calories and / or an increase in ketosis, potentially responsible for dehydration. A poorly hydrated person is very unlikely to have irritable colon diarrhea; only in fasting, as we have said, mucus associated with water can be present.
Other possible intolerances attributable to symptoms of irritable bowel syndrome include that of histamine, salicylates, and hypersensitivity to tyramine-rich foods. Let's not forget that there are potentially irritating, astringent or laxative foods and drinks. While the former are able to promote diarrhea and more rarely constipation (depending on individual susceptibility), the latter promote constipation and the latter cause the loss of stool consistency.
- Among the irritating and stimulating products we distinguish above all: spicy (chilli, pepper and other spices), alcohol and methylxanthines (such as caffeine)
- The astringents are: lemon juice, polished rice, unripe bananas, tea, medlar etc.
- Laxatives include: very high fiber vegetables, warm milk, bran, kiwifruit etc.
Note: there are other active laxative ingredients and are contained in certain products of plant origin.
For foods rich in stimulating nerves it is necessary to make a further clarification, namely that: since it is a disorder probably linked to the emotional-psychological state of the subject, in addition to having a synergistic effect on the contractions of the intestinal smooth muscles, caffeine can aggravate one state of unjustified alertness (anxiety) and act directly even on the primary causes of irritable bowel syndrome.
Behavior
How Does Behavior Affect Irritable Bowel Syndrome?
Very very much. Most people with irritable bowel syndrome are unable to understand the importance of certain spaces, and certain times, throughout the day. This concerns those suffering from diarrhea, which should decrease the frenzy and therefore the constant activation threshold (alert), but above all those who complain of constipation.
Evacuation takes time (extremely subjective) and the intestine (which as we have said is extremely correlated to brain activity) "perceives" the frenzy of everyday life; in constipation, the stimulus is scarcely identifiable and neglecting its onset means postponing it even for many hours. The longer the stool remains in the colon, the harder it becomes due to the re-absorption of water by the mucosa.
Unfortunately, sometimes even the revenue from the necessary time seems not enough because, by artificially modifying the schedules, the risk of ignoring the times of the physiological stimulus increases. This explains why, thanks also to a lower level of general stress, there is often an improvement in symptoms during the holiday period and with the help of anxiolytic drugs.
Note: note how, despite having a totally different onset mechanism, the aggravation of dietary constipation and that of irritable bowel syndrome work in the same way. Therefore, the characterized irritable bowel syndrome alone from constipation, and the so-called idiopathic constipation are not entirely differentiable.
Motor activity
Finally, let's talk about physical motor activity. In addition to not presenting any type of contraindication - however paying attention to the level of body hydration in case of constipation - it boasts a beneficial effect on both constipation and diarrhea. In the first case, it is possible to notice a further articulation of the mechanism. Proceeding in order:
· The natural massage of the intestine induced by physical movement, as well as the diaphragmatic ventilation, favor intestinal transit
Thanks to the secretion of catecholamines - hormones responsible for the hyperexcitability of both smooth and striated muscles - the intestine can benefit from further contractile support.
The effect on diarrhea, on the other hand, is generic and, to tell the truth, it also affects constipation; it is the well known anti-stress mechanism. It too has a polyvalent action, in which the first system purely affects the psychological sphere (playing sports allows you to "switch off") and the second concerns the hormonal release of endorphins (natural opioids secreted by the pituitary gland in the brain).
drugs
After having clarified the role of diet and motor activity in irritable bowel syndrome, it is necessary at least to mention the other possible methods to reduce symptoms and promote the remission of the disorder. At the discretion of the physician, there are drugs that "could" help moderate unwanted manifestations.
Irritable bowel medications
These are: anticholinergics (which decrease intestinal excitability, indicated in case of diarrhea), antidiarrheal (reduce visceral sensitivity, intestinal motility and mucous secretion, indicated in case of diarrhea), antidepressants (for indiscriminate application), prokinetics ( increase intestinal motility, indicated in case of constipation) and serotonergic drugs (intestinal receptor antagonists, indicated in both cases).


























